Emergency thoracotomy
A patient who has sustained truncal trauma but remains unstable or moribund despite adequate resuscitation by way of infusion, chest drainage and ventilation should be considered a candidate for emergency thoracotomy (ET). A penetrating injury anywhere between the nipples laterally, the sternal notch superiorly and the umbilicus inferiorly should be considered to have penetrated the heart till proven otherwise. Ideally ET should be done in a fully equipped operating theatre (if a fully functional operating theatre is available in the A&E department some of the following comments do not apply).
To get the patient to that theatre consider:
-
•Get the ambulance to take direct to theatre and call the surgeons to meet them there
-
•Pass a Foley catheter through the skin incision as far as it will go, inflate the balloon and pull gently back on it to seal any hole.
-
•At the RVH (at present), even after arrest the patient is likely to do better being transported to the operating theatre rather than open in casualty
Indications
The only patients who benefit from thoracotomy in the Emergency Department (as opposed to transferring to a formal operating theatre) are those with cardiac arrest following penetrating or occasionally blunt thoracic or abdominal trauma. These are patients with either cardiac tamponade or exsanguination. They cannot be resuscitated without thoracotomy and the delay in transferring to the operating theatre can decrease the chance of resuscitation or increase the period of cerebral hypoxia. The difference between a patient eventually being able to walk out of hospital by himself rather than being in a vegetative state may be exacerbated by a delay of a matter of minutes in the resuscitative period. In this situation even a non-thoracic trained surgeon can buy time by beginning the incision, performing a pericardotomy and relieving the tamponade. Finger pressure or a Foley catheter may then be enough to control bleeding and allow formal thoracotomy.
Lack of pupillary response is not a contraindication to operation, though it would be an indication for emergency room thoracotomy rather than transfer to an operating theatre. Patients who have shown no signs of life (respiratory activity or pulse) from the time of pick-up will not survive (Champion HR, Danne PD, Finelli. Emergency Thoracotomy; Arch Emerg Med. (1986) 3:95-99). However, as the subtle details of the patient's condition at the scene and during transport are not always available in the heat of the moment, it is difficult to lay down rigid rules for performance of emergency thoracotomy. If a patient seems likely to die from massive haemorrhage or tamponade thoracotomy should be attempted. If your patient survives it is a commendable achievement. If not, you have lost nothing.
Equipment
In general do not attempt ET unless in an operating room equipped with:
-
•surgeons experienced in opening the chest in the right place - each hospital must decide which members of staff are going to be available within minutes to operate. These staff will then require appropriate training.
-
•theatre nurses experienced at thoracotomy
-
•trauma anaesthetists (no specific need for thoracic training as no double lumen tube required, cardiac training useful as pharmacological resuscitation may be important)
-
•an anaesthetic machine and endotracheal intubation set,
-
•anaesthetic drugs, infusions, emergency blood stocks, emergency intravenous and intracardiac drugs
-
•internal and external defibrillation paddles
-
•A thoracotomy instrument set with two rib spreaders (in case clamshell incision)
-
•An instrument to open the sternum. Ideally a mechanical saw but in the middle of the night the nurse may not be able to fit it together. Therefore a Gigli saw and an appropriate sternal bone cutter should be available in addition to any mechanical saw.
-
•Reasonable range of sutures to close wounds in the heart or great vessels e.g. 2/0 Prolene, 3/0 Prolene, 4/0 Prolene (any smaller will be difficult in adverse conditions) and the ubiquitous 2/0 Vicryl for oversewing other bleeding vessel.
-
•Pledget/buttressing material (eg Teflon strips or PTFE) for those sutures
-
•Cardiopulmonary bypass is generally not required in the emergency situation. While the equipment may be easily available, the costs of keeping a team capable of using the equipment makes it unfeasible.
-
•Nylon tapes and "snuggers" are useful for taping the SVC and IVC for inflow occlusion, or for surrounding the hilum in case of major lung laceration.
-
•Adequate suction apparatus for surgeon and anaesthetist
Incision
Incisions are adapted to the circumstances and the track of a weapon, the predicted injuries. Sometimes the presence of a protruding weapon will determine what approach is suitable. ET should be performed with the patient supine. If abdominal injuries are suspected, a separate laparotomy incision can be made in the supine patient without having to reposition him. For the patient who has circulatory collapse after a penetrating injury to the praecordium I prefer a median sternotomy because it gives access to all the major important structures.
Anterior thoracotomy
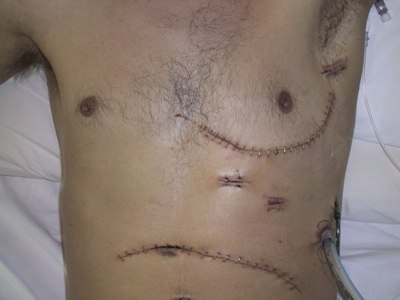
The image on the right is of a left hemiclamshell for a gunshot wound (visible in the axilla).
This incision allows good access to the cardiac ventricles, main pulmonary artery, left hilum and the left lung.
The commonest mistake is to make the incision too low - the heart is higher than you think.
Think of the incision as stage one of a "clamshell"
-
•Mark the fourth cartilage by counting down from the sterno-manubrial angle (2nd cartilage).
-
•A slightly less refined but practical suggestion which has been made is: "when in doubt, find the level of the nipples and join the dots; someone can always come after you to do a cosmetic repair". [Or as a thoracic surgeon from a more disreputable part of the island was heard to remark "if you want to do the job properly .... you shoot them through the second button and open them through the third!"]
-
•Make the incision submammary if possible curling up to the previously marked point on the sternum.
-
•Continue through the intercostal space with the scalpel.
-
•Identify the phrenic nerve and pick up the pericardium in front of it with long (Roberts) artery forceps.
-
•Develop the pericardotomy superiorly and inferiorly. Occlude any laceration with finger pressure.
Access to the heart for definitive repair is poor with this incision and it may need to be converted into a "clamshell" to allow access to the right atrium, aorta, right hilum and lung, or "trapdoor" to approach the arch of the aorta and neck vessels.
"Clamshell"
The anterior thoracotomy can be converted to a "clamshell" (bilateral antero-lateral thoracotomy) incision to allow access to the right atrium, aorta, right hilum and lung.
-
•The anterior thoracotomy is continued across the sternum into the right fourth intercostal space as a mirror image of the initial incision
-
•Use a bone cutter to divide across the sternum. Internal mammary arteries will need to be suture/ligated once a cardiac output has been regained.
-
•Eother place two retractors, one on either side, or a single retractor between the two parts of the sternum. If the incision has been made too low there will be no sternum inferiorly and retraction will be difficult.
-
•If the trauma is obviously right sided the thoracotomy should be performed on that side.
"Trapdoor"
The anterolateral thoracotomy can be transformed into a 'trapdoor' incision
-
•splitting part or all of the sternum
-
•making a second intercostal incsion
-
•elevating the clavicle
-
•or converted to a 'T'shape by splitting the sternum vertically.
Median sternotomy
For the patient who has circulatory collapse after a penetrating injury to the praecordium I prefer a median sternotomy because:
-
•if the patient has collapsed it means that the heart or other major structure has been injured
-
•median sternotomy gives access to all those major structures
-
•the cardiac surgeon is more familiar with that approach
-
•access to hilar vessels is possible using this approach - a sling may be passed round either hilum for emergency control, or the vessels may be controlled within the pericardium.
-
•inflow occlusion (clamping of both SVC and IVC) allows a blood-free field for short periods to allow more accurate repair
-
•the incision can be extended to the neck and allows good proximal control neck vessel injury
-
•the incision can be extended laterally to address lung injuries though virtualy all areas of the lung are accessible through this approach (some surgeons use it as there preferred incision for lung resection)
The disadvantages of median sternotomy are:
-
•it requires an implement to cut bone (bone cutter, Gigli saw, mechanical saw)
-
•access to the descending aorta is difficult
-
•access to posterior chest wall vessels is poor
However, if the life-threatening injury is obviously cardiac, the approach which allows the most direct access is the median sternotomy.
Postero-lateral thoracotomy
In the case of urgent thoracotomy, where resuscitation has been successful and there is more time available for definitive repair of damaged structures, the approach is usually by standard postero-lateral thoracotomy. If the upper abdomen is involved as well as the chest a seventh rib incision allows extension across the costal margin. This gives good access to the upper abdominal vessels (many vascular surgeons approach elective aneurysms from this approach), the stomach and the spleen. Combined chest and hepatic injuries are accessible but the liver is probably better approached from a roof-top incision. A low right side thoracic penetrating injury is likely to involve the liver and after insertion of chest drains it may be wiser to perform laparotomy, the diaphragm being repaired from below. For lower abdominal injuries, less likely to involve major vascular structures, a separate laparotomy is recommended after the thoracotomy has been completed.
Sub-xiphoid pericardotomy
As an alternative to pericardiocentesis, when cardiac injury is suspected, or when the abdomen has been opened before the chest, it has been suggested that a subxiphoid pericardotomy will confirm injury (Miller F, Bond S, Shumate C, Polk H, Richardson J (1986) Diagnostic pericardial window: a safe alternative to exploratory thoracotomy for suspected heart injuries. Arch Surg 122: 605-9). We would advise caution in such an exploration as the subxiphoid incision gives poor access in order to repair a cardiac injury if one is found, and the protective tamponade is lost until suitable access is obtained. Percutaneous echocardiogram is probably a better alternative.
Procedures
There is a limit to the types of procedures which can be performed in the emergency room. Most will be temporising measures until the patient is transferred to an operating room for formal treatment.
-
1.Relief of Cardiac Tamponade:
-
2.Internal cardiac massage,
-
3.Venous access/infusion,
-
4.Control of haemorrhage,
-
5.Cross clamping the descending aorta,
-
6.Pharmacological resuscitation: The tamponaded or contused heart will be 'concussed' for a period of time and may need defibrillation and pharmacological support in addition to internal cardiac massage to maintain a satisfactory output.
-
7.Cardiopulmonary bypass may occasionally be required.
Discontinuation of Resuscitation
Criteria for prompt discontinuation of resuscitation have been well stated by Champion et al. (see reference above) They are:
-
1.Irretrievable anatomic injury. eg ruptured heart
-
2.Failure to volume resuscitate (pH 7.0 - 7.6) within 15 minutes of starting.
-
3.Failure to sustain spontaneous cardiac rhythm and maintain mean systemic blood pressure greater than 50mm, with or without inotropic support within 30 minutes.
Outcome
In any series the outcome of patients undergoing emergency thoracotomy depends on the entry criteria used in selecting patients for that series. In general the patients who survive with reasonable cerebral function are young, previously fit and have had only a short period of circulatory arrest. The minimum requirement is the presence of some sign of life during transit. Patients with blunt trauma do notoriously poorly to the extent that it may be deemed unwise to even consider further measures if standard resuscitation fails. Stab wounds generally fair better than gunshot wounds and 'buckshot' shotgun wounds or high velocity projectiles which have splintered on bone usually produce irreparable damage. The finding of cardiac tamponade in cardiac arrest is a positive prognostic indicator, as are the restriction of injuries to the thorax, singular ventricular injury and successful rapid repair of any defect.
Mattox et al reported survival of 30% following emergency room thoracotomy though most reports are in the region of 5 per cent (Mattox KL, Espana R, Beall CC Jr, Jordan GL Jr. Performing Thoracotomy in the emergency center. J Am Coll Emerg Phys (1974)1:13-17). Of those who survive resuscitation many have prolonged convalescence and cerebral damage. Attempts to use scoring systems to differentiate those likely to survive and those likely to be severely handicapped or to die after prolonged treatment have not been particularly successful. Those patients with a Trauma Score of 1 or 2 have little chance of survival except when the injury is penetrating, though those with a score of 3 or 4 have 9 per cent survival (Fischer RP, Flynn TC, Miller PW, Rowlands BJ. The economics of fatal injury: Dollars and Sense. J Trauma (1985) 25(8):746-750). However, Gaillard et al (Gaillard M, Herve C, Mandin L, Raynaud P. Mortality prognostic factors in chest injury. J Trauma(1990);30(1):93-96) showed that while scoring systems are useful in retrospect for prognosticating in groups of patients, their sensitivity in the individual case is less accurate.
Summary
Provided that experienced personnel are available and accurate assessments have been made there is a place for emergency room thoracotomy. Candidates are patients who have cardiac arrest after trauma, have exhibited signs of life during rapid transit to the emergency room, have not responded to standard resuscitation or who have deteriorated in the emergency room after adequate resuscitation. All other thoracotomies should be performed in the regular operating theatre. Emergency thoracotomy carried out by the inexperienced operator in patients who do not require it must be avoided because of the considerable morbidity and mortality of the procedure.
References of interest:
-
1.Aihara R, Millham FH, Blansfield J, Hirsch EF. Emergency room thoracotomy for penetrating chest injury: effect of an institutional protocol.J Trauma 2001 Jun;50(6):1027-1030
-
2.Branney SW, Moore EE, Feldhaus KM, Wolfe RE Critical analysis of two decades of experience with postinjury emergency department thoracotomy in a regional trauma center. J Trauma 1998 Jul;45(1):87-94 (Denver Health Medical Center, Colorado 80204, USA.)

