Thoracic Epidural - a flawed gold standard

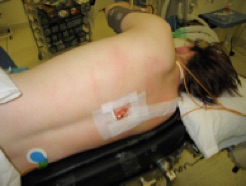
One problem for surgeons is that they take a long time to insert. The introduction of epidurals in our hospital reduced the number of thoracotomies from 3 per day to 2 per list. Bleeding and the risk of paraplegia are real problems with epidurals. We have also had cases cancelled because minor coagulation abnormalities (e.g.Aspirin) have prevented an epidural being attempted, with the inevitable disruption of the surgical list.
Malposition - a recognised complication leading to ineffective block
Ineffective block - often the result of malposition. It is important that this be identified early and treated by reposition or other form of analgesia rather than repeated ineffective "top-ups" by the on-call anaesthetic SHO in the middle of the night The patient will be well into the pain cycle by the time the cavalry arrives in the morning!
Peripheral vaso-dilatation - is a necessary effect of epidural analgesia. it results in hypotension.
Hypotension naturally occurs following insertion of an epidural. To counter this, some anaesthetists automatically start an inotrope when using a thoracic epidural to reduce the incidence of cardiovascular instability in patients who already have a significant degree of cardiovascular co-morbidities. Other anaesthetists compensate for hypotension by over-infusion of fluids. This has the undesirable side effects of oedema and respiratory compromise, particularly following pneumonectomy. There is evidence that the epidural induced hypotension reduces gastric graft blood flow during and after oesophagectomy (Field 2006). Be aware that a patient who is normally hypertensive with a BP of 200/120 is in fact hypotensive at 120/80. At this blood pressure he may not be able to perfuse his kidneys past his renal atherosclerosis or his right gastro-epiploic artery.
Poor urine output - the result of the hypotension and poor perfusion of the kidneys. While it may respond to boluses of fluid most of the said fluid will be retained and will need to be dealt with later. Judicious usage of renal dose inotropes may be more appropriate.
Shoulder tip pain - shoulder tip pain occurs after epidural for thoracotomy and cholecystectomy, and laparoscopy, and obstetric epidural, in most cases being put down to diaphragmatic irritation. This does not explain why it also happens after (open) inguinal hernia repair. In Thoracic surgery it is variously blamed on the irritation of the diaphragm (injection of Marcaine into the diaphragm directly or the pleura via the drains has no effect), apical irritation by the chest drain (still occurs in pneumonectomies where no drain is placed), apical irritation by the surgeon (direct injection of marcaine under the apical pleura has no effect), brachial plexus pain due to positioning of the arm (it occurs regardless of the position of the arm). Injection of the phrenic nerve has been shown to reduce shoulder-tip pain without seriously affecting respiration. A practical way of administering this is to inject the pericardial fat pad with 20mls of Marcaine or Chirocaine.
Adjuvant narcotics - because narcotics are usually incorporated in the infusion, adjuvant narcotics are generally contra-indicated. This makes shoulder tip pain difficult to treat. This problem does not arise where a purely Marcaine epidural is used in conjunction with PCAS narcotic.
Urinary retention - urine retention is so commonly a problem, and urine output so vital in fluid management, NSAID prescription etc, that a urinary catheter is mandatory when a Thoracic epidural is in situ. A true thoracic epidural should not affect bladder function but usually does. In women it may be possible to avoid catheterisation.
Immobilisation - there are perceptions that patients should not mobilise when they have an epidural. This is not the case but it is very difficult to convince nursing staff to mobilise patients.
All of the above are exacerbated in post-pneumonectomy patients in whom fluid balance is very delicate. If fluids are used to counter the vaso-dilatory effect of the epidural there will be an excess of approximately 3000cc. This will recirculate and accumulate on the lungs on day three postop increasing the likelihood of pulmonary oedema which is invariably fatal after pneumonectomy.
Similarly after oesophagectomy, particularly in older patients or those with a cardiac history, where the fluid balance often reaches 7000cc by day three, pulmonary oedema is a danger. In this situation it is wise to have a central line in place and use an inotrope to compensate for the epidural. This will also allow CVP readings and judicious use of diuretics to offload fluid.
